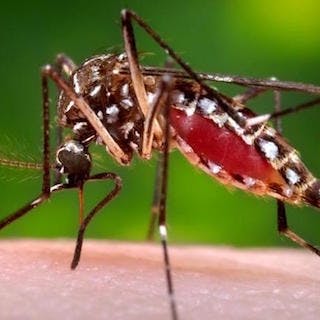
If the spread of the Zika virus does indeed reach epidemic levels, its impact will underscore once more the lethal intersection of class and gender in public health tragedies. The poor always suffer disproportionately when new forms of disease strike; when this poverty is also combined with other kinds of social marginalization, such as gender (or, for instance, sexual minority status in the case of HIV/AIDS) the assault is usually greater than the sum of its parts.
In this case, poverty increases the probability of exposure to the Zika virus carrying mosquito because standing water is a universal feature of poor neighborhoods for two reasons:
One, because water tends to collect easily in the numerous inadvertent receptacles that dot such neighborhoods – the potholes, the empty containers that are saved for possible future use, the rotten tires that decorate poor urban landscapes – almost anything with an open concavity can serve as a home for the water that too seems to appear almost out of nowhere in hot, humid conditions.
Secondly, there is a welcoming home for the Aedes mosquito to thrive in poor areas because, thanks to 24-hour access to piped water still being a distant dream for many such communities, the poor more often need to consciously store water for everyday use.
Being poor is bad enough in this context. But being poor and female is even worse, because it increases the possibility that the outcome – an infection with Zika – will be more devastating than the rash or fever or conjunctivitis that typically describes the infection.
The potential epidemic also underscores the narrow ways in which we tend to describe reproductive health even when we think we are broadening our definition to include much more than contraceptive access. Assured reproductive health means not just the ability to prevent unwanted pregnancies; it also means the right to go through a healthy pregnancy and to end up with delivery that results in a healthy birth. To all the hazards of pregnancy and delivery that poor women worldwide experience, we now need to factor in one more – the possibility that the outcome will be a child that is condemned to a lifetime of poor cognitive development.
If this virus spreads to other parts of the developing world (and the mosquito carrying it is already ubiquitous there, as, for example, the annual epidemic of dengue in India testifies), then the further deterioration of already severely compromised reproductive health is inevitable. But there does not as yet seem to be any sense of alertness to this possibility in countries that are geographically far from the epicenter of the current crisis. The World Health Organization Regional Office for the Americas has been working closely with affected countries since May 2015, but it is already time for even more partners to become involved.
As to what this much-needed heightened and broadened alertness should lead to, one hopes that the easy way out – exhorting women to delay pregnancy or abort pregnancies that might be infected – will not be the standard response. Much more useful will be concerted public health efforts to destroy the mosquito (this will also reduce the incidence of other debilitating illnesses like dengue and chikunguniya) as well as to educate entire families (and not just the women in families) about the dangers of stagnant water.
Most important of all, the cause of decimating the risk of spreading Zika, as well as making the daily lives of poor women a bit easier, will be served by making much stronger efforts to bring water pipes into people’s homes or at least to public spaces in communities and then taking the crucial and currently missing last step of actually having water flow through these pipes for more than the customary few hours each day.
Photo: CDC
Editor’s note: To read more from the author on this topic, visit http://www.epw.in/system/files/pdf/2016_51/9/Postscript_Pages%2093-94.pdf and http://girlsglobe.org/2016/02/12/2-the-zika-virus-a-threat-and-an-opportunity/.